Throughout human history, viruses have played a pivotal role, impacting our societies in various ways. Microscopic adversaries have left a lasting impact on our societies, from the ubiquity of the common cold, which is endemic in many populations, to the vast-reaching pandemics that have rewritten the course of events.
While medical advances have triumphed over certain viral threats, eliminating or containing them, the ever-present possibility of new and potent viral adversaries emerging remains. In today’s hyper-connected world, marked by extensive international travel and commerce, the probability of encountering and spreading novel viruses is magnified.
Therefore, discerning the differences between endemic infections that persist within communities and pandemics that spread across continents is essential. This knowledge, combined with an understanding of virus transmission and disease dynamics, fortifies our readiness against impending viral challenges.
Recent History of Viruses

In recent history, the world experienced an unprecedented event that thrust the global community into uncharted territory – the outbreak of COVID-19. First identified in Wuhan, China, in late 2019, this highly contagious disease caused by the SARS-CoV-2 virus spread rapidly, leading to lockdowns and travel restrictions worldwide.
The scale and impact of this pandemic were unlike anything seen before, as nations grappled with overwhelming healthcare demands, economic upheavals, and the implementation of stringent public health measures. The COVID-19 pandemic highlighted the need for international cooperation and swift action in addressing infectious diseases that transcend borders.
Amid the ongoing challenges of COVID-19, another virus has been garnering attention: Monkeypox. While not a new virus, Monkeypox has been making more frequent appearances in recent years, raising concerns among experts and the international community. Monkeypox, caused by the monkeypox virus (MPXV), has been primarily prevalent in parts of Central and West Africa.
However, its emergence outside of Africa and the occurrence of global outbreaks have ignited discussions about the potential for another global pandemic on the horizon. As scientists and health authorities closely monitor the spread and impact of this disease, the world grapples with the question of whether the next major infectious disease outbreak is closer than we might expect, underscoring the need for robust preparedness and response strategies.
Monkeypox
What is it?
Monkeypox, caused by the monkeypox virus (MPXV), was first identified in monkeys used for research in Denmark in 1958. The virus belongs to the Orthopoxvirus genus in the Poxviridae family, which also includes variola (smallpox), cowpox, and vaccinia viruses.
The first reported human case of monkeypox occurred in the Democratic Republic of the Congo (DRC) in 1970. Since then, monkeypox has been recognized as a disease that can affect both animals and humans.
Source and reservoir hosts:
The natural reservoir of the monkeypox virus is still unknown. However, various small mammals, including squirrels and monkeys, are considered susceptible to infection. These animals might serve as hosts for the virus in the environment, contributing to its transmission.
Outbreaks and geographical distribution:
After the eradication of smallpox in 1980 and the discontinuation of smallpox vaccination, monkeypox began to emerge in central, east, and west Africa. The virus caused localized outbreaks in these regions, leading to concerns among health authorities.
Additionally, sporadic cases of monkeypox have been reported in other parts of the world, including North America, Europe, and Asia, likely due to international travel, imported animals, or close contact with infected individuals or animals. A global outbreak occurred in 2022–2023, primarily affecting gay, bisexual, and other men who have sex with men and spreading through sexual networks.
The World Health Organization declared the global outbreak of monkeypox a public health emergency of international concern in July 2022. The WHO has published a strategic preparedness and response plan for monkeypox and continues to focus on surveillance, diagnostics, risk communication, and community engagement to stop the outbreak and eliminate human-to-human transmission of monkeypox.
Difference to COVID-19 in background and origin:
The origins and natural reservoirs of the two viruses differ, with COVID-19 suspected to have zoonotic origins, possibly originating from bats, and monkeypox’s natural reservoir still remaining unknown.
Causative Agents and Transmission
Monkeypox can spread from person to person through direct contact with infectious skin or other lesions. This includes face-to-face contact, skin-to-skin contact, mouth-to-mouth contact, and contact with respiratory droplets or short-range aerosols from prolonged close contact.
The virus enters the body through broken skin, mucosal surfaces, or the respiratory tract. It can also spread from infected animals to humans through bites, scratches, or during activities such as hunting, skinning, or cooking animals. Transmission can also occur through contact with contaminated objects.
Factors affecting transmission rates:
Several factors influence the transmission rates of monkeypox. Firstly, close contact with infected animals or humans increases the risk of transmission. Additionally, activities that involve handling or processing infected animals, such as hunting and cooking, can facilitate the transmission of the virus.
Furthermore, the presence of infected animals in the environment and the interaction between animal populations and humans play a role in the spread of the virus. Factors like population density, healthcare infrastructure, and public health measures also influence the rate of transmission during outbreaks.
Differences to COVID-19 in transmission:
In contrast to monkeypox, COVID-19 is caused by the SARS-CoV-2 virus, which is a novel coronavirus. The transmission of COVID-19 primarily occurs from person to person through respiratory droplets produced when an infected individual talks, coughs, or sneezes.
It can also spread by touching surfaces contaminated with the virus and then touching the face. Unlike monkeypox, there is no evidence of COVID-19 transmission from animals to humans, although the virus may have zoonotic origins.
COVID-19 has demonstrated a higher rate of human-to-human transmission compared to monkeypox, contributing to its rapid global spread and the need for strict public health measures to contain its transmission.
Additionally, COVID-19 has been associated with a broader range of clinical manifestations, affecting the respiratory system primarily, while monkeypox typically presents with a characteristic rash and lymphadenopathy.
Incubation Period and Symptoms
The incubation period for monkeypox is typically around 7 to 14 days, but it can range from 5 to 21 days. Following exposure to the virus, individuals may remain asymptomatic during this period.
Once symptoms appear, they usually begin within a week, but the onset can take up to 21 days after exposure. The incubation period for COVID-19 ranges from 2 to 14 days, with an average of about 5 to 6 days.
Unlike monkeypox, which typically presents symptoms within a week of exposure, COVID-19 symptoms may appear sooner after exposure. Additionally, COVID-19 has a broader range of incubation periods, with some individuals showing symptoms within just a few days after exposure.
Common clinical manifestations:
Monkeypox presents with a variety of symptoms, some of which are similar to smallpox, but generally milder. Common clinical manifestations include fever, rash, sore throat, headache, muscle aches, back pain, low energy, and swollen lymph nodes.
The rash is a characteristic feature of monkeypox and typically starts as flat sores that develop into fluid-filled blisters. These lesions may be itchy or painful and eventually crust over before falling off as scabs.
COVID-19 primarily affects the respiratory system and commonly presents with symptoms like fever, cough, shortness of breath, fatigue, muscle or body aches, headache, loss of taste or smell, sore throat, and congestion. While both monkeypox and COVID-19 may cause fever and fatigue, respiratory symptoms, loss of taste and smell, and congestion are distinctive features of COVID-19 not typically seen in monkeypox.
Severity and complications:
The severity of monkeypox can vary, with most cases being mild and self-limiting. However, in some individuals, the disease can take a more severe course.
Complications may arise, especially in those with weakened immune systems or underlying health conditions. These complications can include secondary bacterial infections, pneumonia, corneal infection leading to vision loss, painful swelling of the rectum, inflammation of the brain (encephalitis), heart (myocarditis), and other organs.
Severe cases can result in death, but the fatality rate for monkeypox is generally lower than that of smallpox. COVID-19 can range in severity from mild to severe, with some individuals experiencing no or mild symptoms and others developing severe pneumonia and acute respiratory distress syndrome (ARDS).
The risk of severe illness is higher in older adults and those with underlying health conditions. Unlike monkeypox, COVID-19 can also cause systemic complications affecting various organs, including the heart, kidneys, and blood vessels.
Diagnosis and Testing
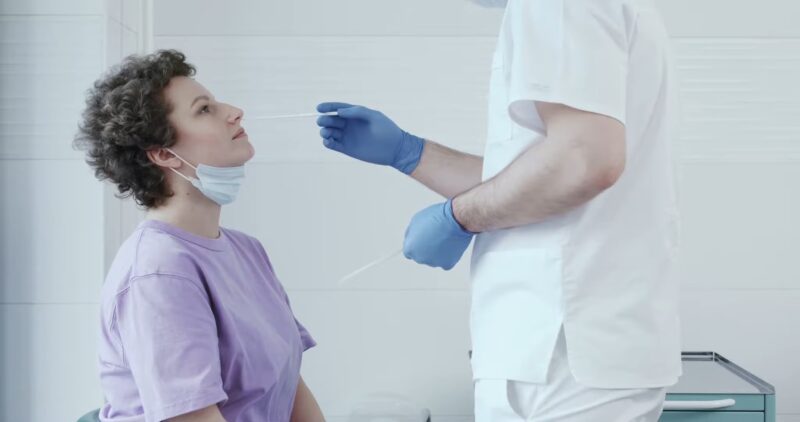
Laboratory tests and techniques:
The diagnosis of monkeypox is typically confirmed through laboratory tests and techniques. Polymerase chain reaction (PCR) assays are commonly used to detect the monkeypox virus’s genetic material in patient samples, such as swabs from skin lesions or respiratory secretions.
Additionally, enzyme-linked immunosorbent assays (ELISA) or other serological tests can identify antibodies against the virus in the patient’s blood, indicating a past or current infection. These laboratory tests play a critical role in distinguishing monkeypox from other similar diseases and confirming the diagnosis.
COVID-19 diagnosis also relies on laboratory tests, but the methods differ from those used for monkeypox. The primary diagnostic test for COVID-19 is the molecular PCR test, which detects the presence of SARS-CoV-2 genetic material in respiratory specimens.
Additionally, rapid antigen tests are used for rapid screening, although they may have lower sensitivity compared to PCR tests. Serological tests, similar to those used for monkeypox, can detect antibodies against SARS-CoV-2 in blood samples, indicating a previous infection.
Differential diagnosis from other diseases:
Monkeypox shares clinical features with other diseases, such as chickenpox (varicella) and smallpox (variola). Therefore, it is essential to differentiate monkeypox from these diseases and other skin conditions that present with similar rashes.
Differential diagnosis is based on clinical presentation, patient history (e.g., recent travel to monkeypox-endemic regions), and laboratory test results. Distinguishing monkeypox from other infectious diseases is crucial for appropriate patient management and public health measures.
Distinguishing COVID-19 from other respiratory illnesses is crucial, as the symptoms may overlap with those of influenza, common colds, and other viral respiratory infections. COVID-19’s distinctive features, such as loss of taste or smell, and the presence of characteristic lung abnormalities on chest imaging, can aid in the differential diagnosis.
Real-time PCR testing remains the gold standard for diagnosing COVID-19 and ruling out other respiratory diseases.
Public Health Response

Public health measures during outbreaks
During monkeypox outbreaks, public health authorities implement various measures to contain the spread of the virus. These measures may include quarantine and isolation of infected individuals, travel restrictions, and public health advisories to raise awareness about the disease and its modes of transmission.
Health authorities may also provide guidance on personal protective measures, such as wearing masks and practicing good hand hygiene, to reduce the risk of transmission. The public health response to COVID-19 has been on a much larger scale due to its global pandemic status.
Governments and health organizations worldwide have implemented various measures, including lockdowns, social distancing guidelines, mandatory mask-wearing, travel restrictions, and mass testing and vaccination campaigns. The impact of COVID-19 on public health and healthcare systems has been far-reaching, requiring coordinated efforts at national and international levels.
Surveillance and contact tracing
Surveillance systems are crucial in monitoring monkeypox outbreaks and identifying new cases. Health agencies work to track and record cases, identify clusters of infections, and investigate potential sources of transmission.
Contact tracing is an essential component of outbreak control, as it helps identify individuals who may have been exposed to the virus and allows for early detection and containment of additional cases.
COVID-19 surveillance and contact tracing have been challenging due to the highly transmissible nature of the virus and its wide-ranging clinical presentations. Rapid and widespread testing has been essential in identifying and isolating cases, as well as tracing and testing close contacts to curb transmission.
Technology, such as digital contact tracing applications, has also been used to augment traditional contact tracing efforts.
Vaccine development and availability
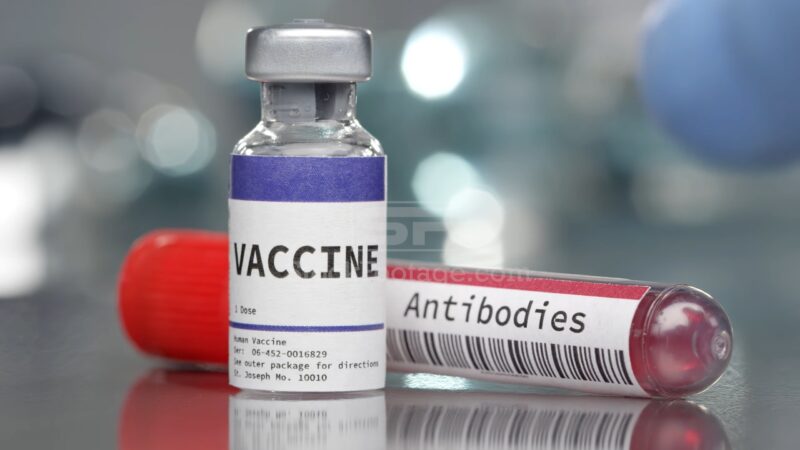
Vaccine development for monkeypox is an ongoing area of research. Several experimental vaccines have shown promise in animal studies and early-phase clinical trials.
However, no licensed vaccine specifically targeting monkeypox is currently available. The development of an effective and safe monkeypox vaccine remains a priority, considering the potential impact of the virus on public health.
Antivirals such as tecovirimat, originally developed to treat smallpox, have been used to treat Mpox. Unlike monkeypox, COVID-19 has seen unprecedented global efforts to develop and distribute vaccines.
Several vaccines against SARS-CoV-2 have been developed and authorized for emergency use in record time. Mass vaccination campaigns have been launched worldwide to curb the spread of the virus and protect vulnerable populations.
The availability of multiple vaccines has been instrumental in increasing global vaccination rates and reducing the impact of COVID-19 on public health.
Case Fatality Rate and Mortality
Fatality rates in different outbreaks:
The case fatality rate (CFR) for monkeypox can vary in different outbreaks and settings. Overall, monkeypox has a lower CFR than its close relative, smallpox.
In some outbreaks, the CFR has been reported to be less than 1%, indicating that the majority of cases result in recovery. However, in specific populations or regions with limited access to healthcare, the CFR may be higher.
The severity of monkeypox and the outcome of individual cases can be influenced by factors such as the age and health status of the affected individuals, access to medical care, and the availability of supportive treatments. COVID-19 has demonstrated a higher overall CFR compared to monkeypox.
The CFR for COVID-19 varies widely across different regions and populations, with some areas experiencing a higher burden of severe cases and deaths. The CFR for COVID-19 is generally higher in elderly individuals and those with pre-existing health conditions, including cardiovascular disease, diabetes, and respiratory conditions.
However, it is important to note that CFR can vary over time and with the availability of healthcare resources.
Vulnerable populations:
Certain populations are more susceptible to severe outcomes from monkeypox infection. Vulnerable groups include children, pregnant individuals, and those with weakened immune systems or underlying health conditions.
In these groups, monkeypox can lead to more severe disease and a higher risk of complications. Additionally, individuals with no prior exposure to the monkeypox virus or smallpox vaccination may be at a higher risk of infection and severe disease if exposed to the virus.
COVID-19 has been particularly severe in certain vulnerable populations. Older adults, especially those residing in nursing homes or long-term care facilities, have been at a higher risk of severe illness and death from COVID-19.
Individuals with underlying health conditions, such as hypertension, obesity, and diabetes, also face an elevated risk of severe outcomes. Immunosuppressed individuals and those with compromised immune systems due to medical conditions or treatments are more susceptible to severe COVID-19.
Long-Term Effects and Recovery
Understanding post-recovery complications:
For individuals who recover from monkeypox, there may be potential long-term effects and complications. While the majority of cases resolve without severe consequences, some survivors may experience lingering effects.
Common post-recovery complications include scarring from the rash and skin lesions, especially if the lesions were extensive or located in sensitive areas. Scarring can have both physical and psychological impacts on individuals.
COVID-19 has been associated with a range of post-recovery complications, often referred to as “long COVID” or “post-acute sequelae of SARS-CoV-2 infection” (PASC). Long COVID can affect individuals who had mild, moderate, or severe COVID-19, and even those who had asymptomatic infections.
Common long-term effects include persistent fatigue, shortness of breath, brain fog, chest pain, joint pain, and loss of taste or smell. Some individuals with long COVID experience a slow and gradual recovery, with symptoms persisting for weeks or even months after the initial infection.
Impact on survivors’ health:
In some cases, severe monkeypox infections can lead to complications affecting various organs, such as the eyes, respiratory system, and nervous system. Survivors who experienced severe disease may face long-term health challenges related to these complications.
For instance, ocular complications can affect vision, respiratory complications may lead to chronic respiratory problems, and neurological complications can result in long-lasting neurological symptoms. Long COVID can have a profound impact on survivors’ health and quality of life.
Individuals with long COVID may face challenges in performing daily activities, returning to work, or resuming physical activities. The lingering effects of the disease can lead to a reduced overall quality of life and require ongoing medical management and support.
Economic and Societal Impact

Localized outbreaks and economic consequences:
Monkeypox outbreaks are typically localized, meaning they occur in specific regions or communities. While these outbreaks can have significant public health implications for affected areas, the economic consequences are generally limited compared to a global pandemic.
Local economies may experience disruptions during outbreaks due to measures like quarantine, isolation, and travel restrictions, which can affect businesses, trade, and tourism. However, the impact on the broader national or global economy is typically less pronounced than a widespread pandemic.
COVID-19, as a global pandemic, has had far-reaching economic consequences on a global scale. Lockdowns, business closures, and travel restrictions imposed to control the spread of the virus have significantly impacted the global economy.
Industries such as travel, hospitality, and retail have been severely affected, leading to job losses and economic downturns in many countries. Governments and international organizations have implemented extensive financial stimulus packages to support economies during the pandemic.
Social stigma and fear:
During monkeypox outbreaks, there can be instances of social stigma and fear surrounding the disease. Misinformation or lack of understanding about monkeypox may contribute to unfounded fears and stigmatization of individuals affected by the virus.
Stigmatization can result in social isolation and discrimination against infected individuals and their families. Public health authorities and community leaders play a crucial role in addressing misconceptions, disseminating accurate information, and promoting empathy and support for affected individuals.
COVID-19 has also been associated with widespread fear and social stigma. As the virus spread rapidly across the globe, individuals from affected regions or with a history of COVID-19 infection may have experienced discrimination or stigmatization.
The stigma surrounding the virus has been fueled by misinformation, xenophobia, and prejudice. Such stigma can deter people from seeking medical care or adhering to public health measures, hindering efforts to control the spread of the virus.
Prevention and Control Measures

Vaccination and its efficacy:
Currently, there is no specific licensed vaccine available for monkeypox. However, research and development efforts are ongoing to create an effective vaccine against the monkeypox virus.
Experimental vaccines have shown promise in animal studies and early-phase clinical trials, but their efficacy and safety in large-scale human populations are still being evaluated. Once a safe and effective vaccine is developed and approved, it could play a critical role in preventing monkeypox outbreaks and protecting vulnerable populations.
Unlike monkeypox, several vaccines have been developed and authorized for emergency use to prevent COVID-19. Vaccines from different manufacturers have demonstrated high efficacy in preventing severe disease, hospitalization, and death.
Vaccination campaigns have been implemented worldwide to immunize populations and achieve herd immunity, contributing to the control of the pandemic. Continuous monitoring of vaccine effectiveness and safety is conducted by health authorities to optimize the response.
Prevention strategies during outbreaks:
During monkeypox outbreaks, prevention strategies focus on breaking the chain of transmission. Public health measures include early case detection, isolation of infected individuals, and contact tracing to identify and monitor individuals who may have been exposed to the virus.
Quarantine measures may be implemented to limit further spread. Additionally, health authorities may promote public awareness campaigns to educate the population about the disease’s modes of transmission and the importance of personal protective measures, such as wearing masks and practicing good hand hygiene.
Surveillance systems are essential for monitoring the outbreak’s progress and implementing timely control measures. COVID-19 prevention strategies have been broader and more complex due to the global scale of the pandemic.
Along with vaccination efforts, prevention measures have included widespread testing, contact tracing, travel restrictions, and social distancing guidelines. Lockdowns and business closures were also implemented during peak outbreaks to reduce virus transmission. Mass public health campaigns emphasized the importance of mask-wearing, maintaining physical distance, and avoiding large gatherings to curb viral spread.
Additionally, advances in digital technology facilitated the development of contact-tracing apps to supplement manual contact-tracing efforts.
Last Words
Viruses have been and will continue to be a fundamental aspect of human existence, shaping our lives and societies in profound ways. The COVID-19 pandemic exposed the vulnerabilities and complexities of global health systems and demonstrated the imperative of international collaboration in combating infectious diseases.
The resurgence of Monkeypox and its potential for global impact have underscored the importance of ongoing research and vigilance in understanding and controlling infectious diseases. By investing in public health infrastructure, fostering international cooperation, and remaining steadfast in scientific advancements, humanity can better equip itself to navigate the uncertainties of infectious diseases and protect global health.
Preparedness, knowledge, and a united global effort are essential components in safeguarding human well-being and building a resilient future in the face of emerging viral threats.
